Advanced Therapies for Overactive Bladder
Sudden bladder urges or leakage? Nighttime bathroom breaks?
Always have to go?
Bladder control problems affect tens of millions of people every day. If you’re one of them, talk to your doctor!
Overactive bladder (OAB) refers to a combination of urgency, frequent urination, nighttime voiding, and sometimes leakage while trying to reach the bathroom (urge incontinence).
Most women with overactive bladder have become familiar with the option of medications (remember those TV commercials: “gotta go, gotta go?”). But what about women seeking non-medication treatments for their OAB symptoms, or for women who have failed to respond or experienced side effects?
Today women have an impressive array of options, and our center has played a role in a great deal of research for this condition. We’ve helped investigate new OAB medications, participated in some of the first clinical studies of Botox for the bladder, and currently treat a large number of women with InterStim sacral nerve stimulation and acupuncture-based nerve stimulation (“PTNS”).
If the usual medications and exercises have failed to improve your bladder control, don’t give up! Advanced treatments for this women’s health condition have improved at a fast pace, and our patients today are reaping the benefits.
Remember: While incontinence is more common as we age, it is not a normal part of aging.
Do I have OAB? Some clues to consider
- Frequent urination: “I’m in the bathroom all the time”
- Urgency: sudden desire to urinate, reduced ‘warning time’
- Urge incontinence: leakage with a bladder urge, often occurring on the way to the bathroom
- Nighttime urination (“nocturia”): up more than 1-2 times per night
- Bathroom mapping: always planning and finding the next bathroom?
Treatments for Overactive Bladder
Botox for the Bladder
Botox is an effective treatment for overactive bladder (OAB) symptoms when someone cannot continue taking OAB medicine pills due to side effects or when the pills are not helping enough.
Botox treatments are typically performed in the office after placing numbing medicine in the bladder and urethra. A small camera (cystoscope) is then placed through the urethra and into the bladder, and the Botox medicine is injected into the wall of the bladder in several spots. Treatments take a matter of minutes, and patients often experience improvement in their urinary urgency, frequency, and urge leakage for an average of 6 months. This allows many women to trade taking bladder control pills every day for Botox treatments twice a year.
Fun Fact: Our center was involved in the pivotal trials leading to FDA approval for Botox, allowing this therapy to become a worldwide success!
InterStim Sacral Neuromodulation: The “Pelvic Pacemaker”
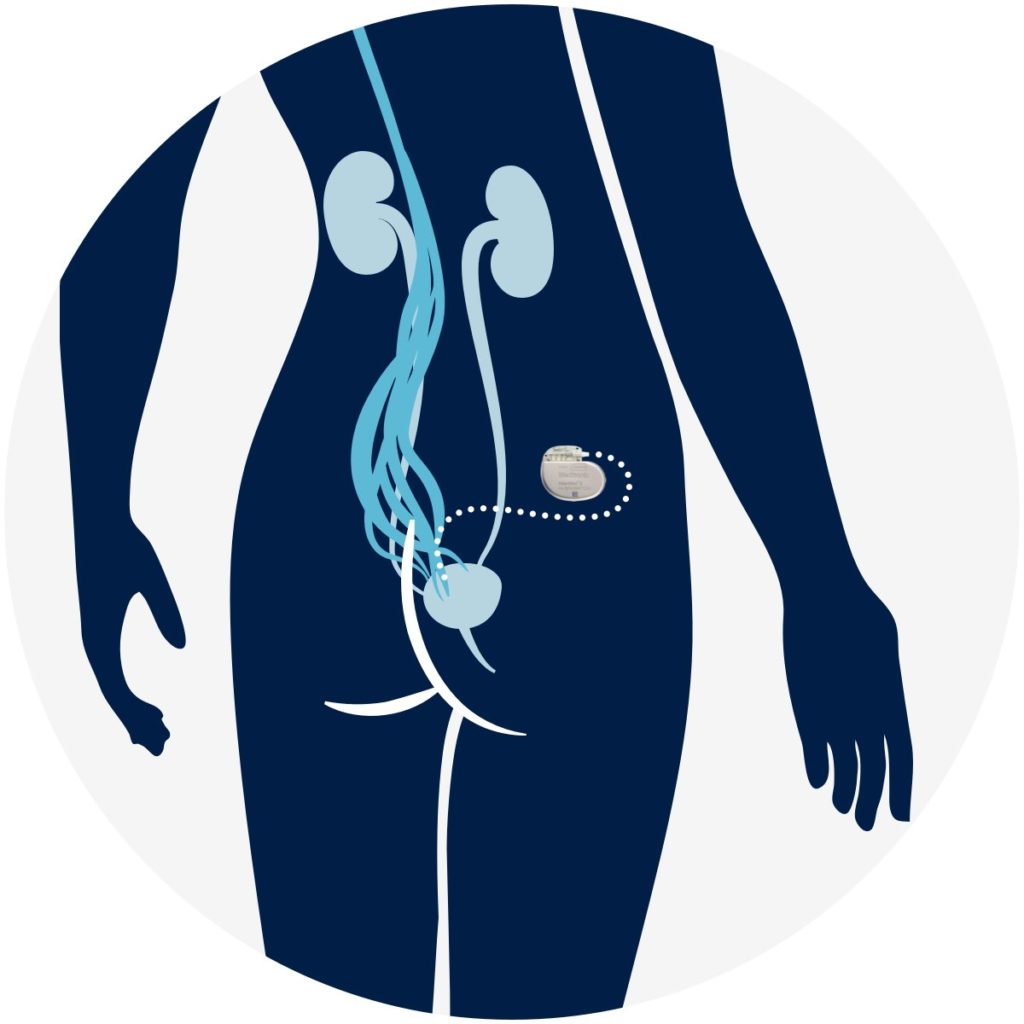
Unlike medications that typically work by relaxing the muscles in the bladder, the Medtronic InterStim system targets the nerves that control your bladder to help restore normal bladder function. First, you will com into the office for a simple in-office test, and if you bladder function improves, the permanent stimulator is placed during a quick out-patient procedure. The Medtronic therapy has been proven for over 25 years with the most advanced technology on the market for sacral nerve stimulation for our patients and we have been performing this procedure for nearly 20 years!
Percutaneous Tibial Nerve Stimulation (PTNS): “Acupuncture for the Bladder”
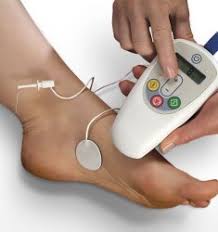
PTNS is a highly effective treatment for women with Overactive Bladder symptoms involving mild electrical stimulation of the “tibial nerve” which is located near the outside of the ankle. Stimulation of this nerve eventually travels to the sacrum (below the spine) where bladder control is impacted. PTNS has become an incredibly popular option in our practice over the past few years for several reasons: it works very effectively for most women, it’s well tolerated and performed in a 30 minute session, and it involves no medication. Most insurers cover PTNS treatments for women who have not successfully responded to ‘first line’ therapies such as OAB medication.
Coming Soon: More Implantable Therapies
The success of PTNS has led to several new innovations, now in development. Our center is currently participating in a study evaluating an implantable stimulator inserted through a small incision near the ankle, allowing for constant stimulation of the tibial nerve. Whether new implantable therapies will match the success of PTNS remains to be seen, but in the meantime our team is excited about this quickly growing area of women’s pelvic health. Treating OAB in the near future may involve no medications at all, perhaps replaced with implantable chips, even better forms of Botox, or other innovations. Wherever the ball is bouncing, our team is always committed to staying on the cutting edge.
Who We’ve Helped
Dr. Sand is always caring, informative, and includes me in the decision making process of my own medical treatment. He listens to what I have to say, never becoming impatient, and is always a pleasure to be around. I have the highest confidence in Dr. Sand and have referred many people to him over the years. A better doctor you will not find.
Before my procedure, I was unable to walk across the room without pain and discomfort due to my prolapse. In short, your care and this procedure were life-changing. I feel great and I thank Dr. Rostami and her team so much!
My procedure was a repeat surgery and involved a high level of complexity. This was the reason I traveled from out-of-state to specifically see Dr. Goldberg. I felt I couldn’t be in better hands and am delighted with my recovery.
Contact Us
Let’s get you feeling like yourself again.
From scheduling a telemedicine consultation to helping you arrange travel before and after your treatment, we are here to support you at every step. Reach out with questions or to get started.